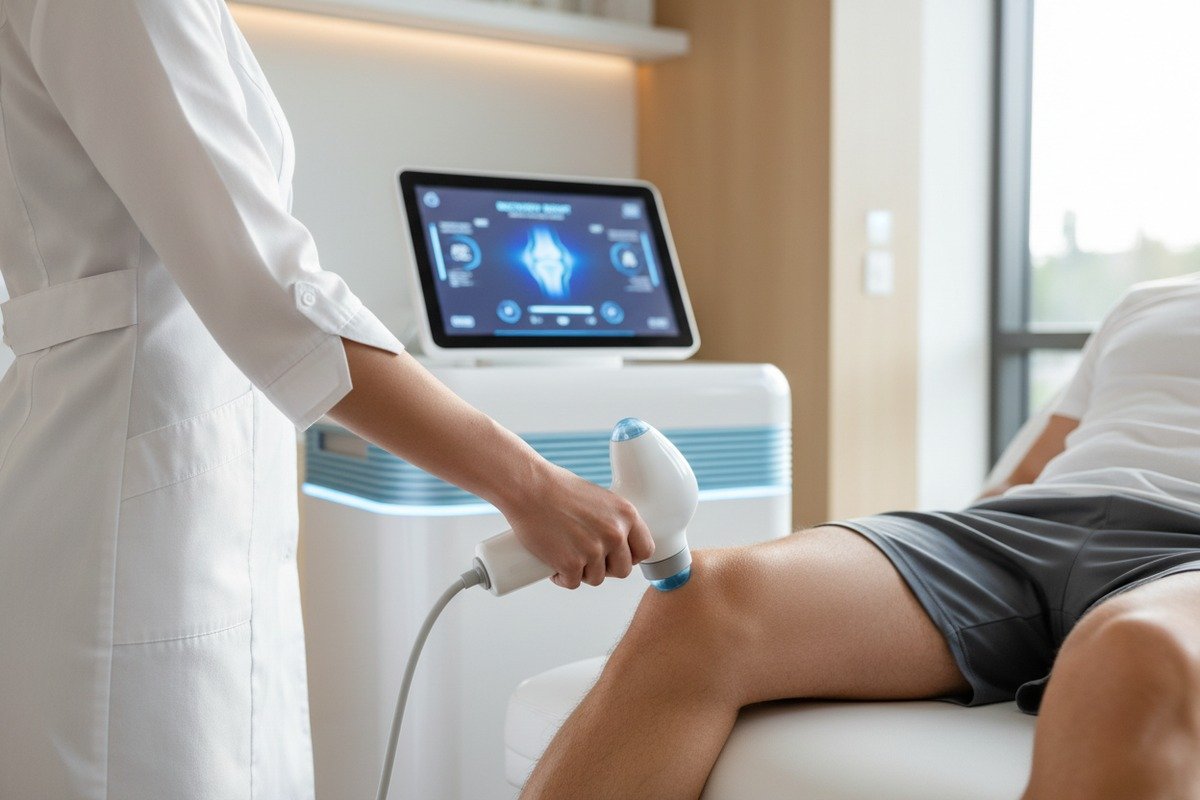
Every week, our production team receives inquiries from clinic owners asking the same question: will this technology actually help patients heal faster after surgery Lysholm scores 1? The frustration is real. You invest in expensive equipment, train your staff, and then wonder if the results will justify the cost.
Shockwave therapy shows modest but measurable benefits for postoperative recovery. Clinical studies demonstrate improved functional outcomes, enhanced blood flow, reduced inflammation, and accelerated tissue regeneration. However, effectiveness varies by surgical procedure, treatment technique, and protocol parameters, making proper device selection and standardized application essential for optimal results.
In this article, we will examine the clinical evidence, safety considerations, and practical factors you need to evaluate before integrating shockwave therapy into your recovery protocols.
How can I be sure shockwave therapy actually speeds up my clients' post-surgery healing?
When we calibrate our shockwave devices on the production line, we test them against specific biological markers surgical scar healing 2. But lab results only tell part of the story. What really matters is whether your patients experience faster, more complete healing in real clinical settings.
You can verify shockwave therapy's effectiveness through measurable functional improvements, typically seen in Lysholm scores and tissue healing assessments. A 2025 meta-analysis of ACL reconstruction patients showed a 3.72-point functional improvement. Longer follow-up periods consistently demonstrate better outcomes, with full benefits appearing 8-12 weeks post-treatment.

Understanding the Biological Mechanisms
Shockwave therapy works through several interconnected pathways. First, mechanical pressure waves stimulate angiogenesis 3. This means new blood vessels form in the treated area. More blood vessels equal better oxygen and nutrient delivery. Tissues with poor natural blood supply, like tendons and ligaments, benefit most from this effect.
Second, the therapy modulates inflammation. Surgery triggers necessary inflammation, but too much slows healing. Shockwave treatment helps tissues transition from inflammation to repair more efficiently. This biological shift is critical for recovery timelines.
Third, stem cell recruitment occurs at the treatment site. The mechanical stimulation signals stem cells to migrate and multiply. These cells rebuild damaged tissue. Research confirms enhanced stem cell signaling in tendons, ligaments, and bone following treatment.
What the Clinical Data Shows
The strongest evidence comes from ACL reconstruction studies 4. Researchers analyzed six studies, including five randomized controlled trials. Here is what they found:
| Outcome Measure | ESWT Result | Clinical Significance |
|---|---|---|
| Lysholm Score | +3.72 points improvement | Modest functional benefit |
| IKDC Score | No significant difference | Limited evidence |
| Pain (VAS) | No significant difference | Immediate relief varies |
| KT-1000 Stability | No significant difference | Structural impact unclear |
These numbers deserve context. A 3.72-point improvement on a 100-point scale is small but measurable. Importantly, focused ESWT outperformed radial ESWT consistently. This tells us technique matters significantly.
Why Follow-up Duration Matters
Studies with longer follow-up periods show better results. Why? Tissue regeneration takes time. Collagen synthesis and remodeling do not happen overnight. Patients report immediate pain relief due to nerve modulation, but true functional improvement requires 8-12 weeks.
For fracture healing 5, the data is encouraging. A systematic review found 72% union rates in nonunion patients. When used alongside surgical fixation for acute fractures, researchers observed a 46% reduction in nonunion risk.
What are the clinical benefits of using shockwave therapy for my patients' surgical scar healing?
Our engineers have found that scar tissue responds differently to various energy settings. Through years of testing and feedback from our international partners, we have learned that scar treatment requires specific protocols distinct from general pain management applications.
Shockwave therapy benefits surgical scar healing by breaking down dense collagen fibers, stimulating healthy tissue regeneration, and improving local blood circulation. Treatment promotes collagen remodeling, reduces adhesions that restrict movement, and decreases scar tissue thickness. Patients typically experience improved flexibility and reduced tightness within several treatment sessions.

How Scar Tissue Forms and Why It Matters
After surgery, your body produces collagen rapidly to close wounds. This emergency repair creates dense, disorganized tissue. Unlike healthy tissue, scar tissue lacks elasticity. It can restrict movement, cause pain, and create adhesions between tissue layers.
Shockwave therapy addresses this problem mechanically. The pressure waves break apart dense collagen bundles. This controlled microtrauma triggers the body to rebuild with more organized tissue. The result is softer, more flexible scar tissue.
The Cellular Response to Treatment
When shockwaves reach scar tissue, several things happen:
| Cellular Effect | Timeline | Patient Benefit |
|---|---|---|
| Collagen fiber disruption | Immediate | Reduced tissue density |
| Inflammatory response | 24-48 hours | Healing cascade activation |
| Fibroblast stimulation | 1-2 weeks | New collagen production |
| Tissue remodeling | 4-8 weeks | Improved flexibility |
The treatment also increases growth factor expression. These chemical signals guide tissue repair. Studies show elevated levels of TGF-beta and VEGF following shockwave application.
Preventing Adhesion Formation
Adhesions form when scar tissue connects structures that should remain separate. This causes pain and limits mobility. In our experience supplying clinics across Europe and North America, practitioners report that early shockwave intervention reduces adhesion severity.
The key is timing. Treatment works best during the remodeling phase of healing. Starting too early risks disrupting initial wound closure. Starting too late means the scar has already matured into rigid tissue.
Beyond Visible Improvements
Internal scars matter too. Deep tissue adhesions affect function even when surface healing looks normal. Shockwave therapy penetrates beyond skin level. Depending on energy settings, treatment can reach muscles, fascia, and connective tissue.
Some practitioners combine shockwave therapy with manual techniques. The mechanical softening from shockwaves makes subsequent manipulation more effective. This hybrid approach often produces better results than either treatment alone.
Are there any safety risks I should consider before adding shockwave therapy to my recovery protocols?
At our facility, every device undergoes rigorous safety testing before shipment. We have seen the consequences when clinics use poorly calibrated equipment. Patient safety depends on both device quality and proper application protocols.
Safety risks of shockwave therapy include temporary pain during treatment, localized bruising, skin redness, and numbness. Contraindications include treatment over blood clots, tumors, infections, growth plates in children, and pregnancy. Device quality, operator training, and adherence to established protocols significantly reduce risk. Most adverse effects are mild and self-limiting.
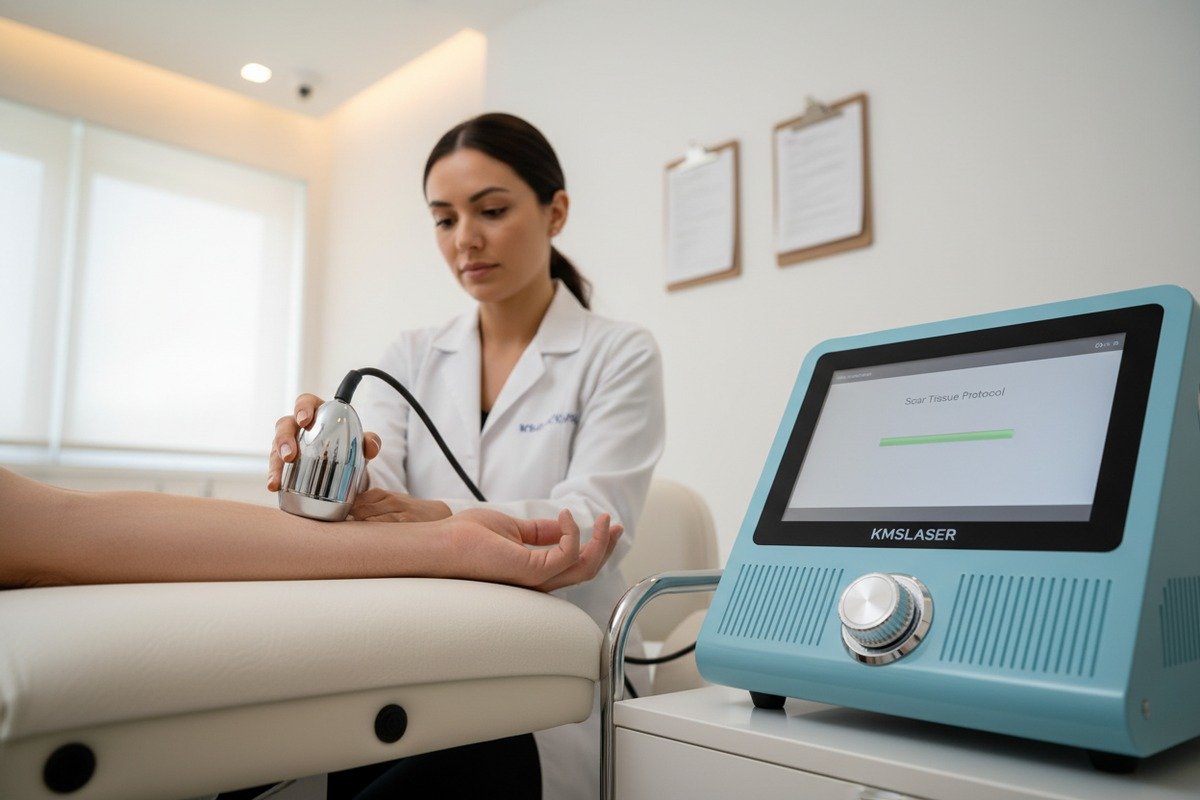
Common Side Effects and Their Management
Most patients tolerate shockwave therapy well. However, some side effects occur regularly:
| Side Effect | Frequency | Duration | Management |
|---|---|---|---|
| Treatment discomfort | Common | During session | Adjust energy level |
| Skin redness | Common | 1-2 hours | No treatment needed |
| Bruising | Occasional | 3-7 days | Ice application |
| Numbness | Rare | 24-48 hours | Monitor and reassure |
| Swelling | Occasional | 1-3 days | Elevation, ice |
These effects result from the mechanical nature of treatment. Pressure waves cause minor tissue disruption. This is intentional and necessary for therapeutic benefit. The key is distinguishing normal reactions from complications.
Absolute Contraindications
Certain conditions make shockwave therapy dangerous. Never treat over:
- Blood clots or thrombophlebitis
- Malignant tumors
- Active infections
- Open wounds
- Growth plates in pediatric patients
Pregnancy also contraindicates treatment. The effects of pressure waves on fetal development remain unstudied. Caution requires avoiding treatment entirely during pregnancy.
Relative Contraindications and Precautions
Some situations require careful consideration rather than absolute avoidance. Patients on blood thinners may bruise more easily. Reduce energy levels and monitor closely. Metal implants do not necessarily prevent treatment, but avoid direct application over superficial hardware.
Patients with nerve disorders need special attention. Shockwave therapy affects nerve function temporarily. In patients with existing neuropathy, this effect may be unpredictable.
Device Quality and Operator Competence
Our quality control team has identified a troubling pattern. Low-quality devices produce inconsistent energy output. One pulse might deliver adequate energy while the next delivers significantly more or less. This variability creates unpredictable treatment effects.
Operator training matters equally. Understanding anatomy, proper positioning, and energy titration prevents complications. Untrained operators may treat inappropriate areas or use excessive energy.
When evaluating equipment, ask suppliers about energy consistency testing. Request documentation of pulse-to-pulse variability. Quality manufacturers provide this data readily.
How do I find a reliable shockwave machine manufacturer that meets my brand's quality standards?
Through our years of exporting to the US, Canada, and Europe, we have learned what separates reliable suppliers from problematic ones. The questions you ask during evaluation predict the partnership quality you will receive.
To find a reliable shockwave machine manufacturer, evaluate their quality control documentation, request technical specifications for energy output consistency, verify regulatory certifications, assess their after-sales support capabilities, and test sample units before committing to orders. Manufacturers should provide user profile storage capacity details, power interruption data protection features, and customization options for your market requirements.

Essential Technical Questions to Ask
Start with performance specifications. Request documentation showing:
| Specification | Why It Matters | Acceptable Standard |
|---|---|---|
| Energy output range | Treatment versatility | 0.01-0.5 mJ/mm² |
| Pulse frequency | Protocol flexibility | 1-22 Hz |
| Pulse-to-pulse consistency | Treatment predictability | ±5% variance |
| Penetration depth | Deep tissue access | 0-60mm adjustable |
| Treatment head options | Application variety | Minimum 3 heads |
Beyond these basics, ask about user interface features. How many user profiles can the machine store? This matters for multi-practitioner clinics. Can you easily recall patient-specific protocols? Time saved on settings adjustment improves clinic efficiency.
Power Interruption Protection
Here is a question many buyers forget: What happens during power failure? Ask your supplier: Does the machine support data protection during power interruption? How long does this protection last? Quality machines save treatment data and settings automatically. Lower-quality units lose everything, requiring complete reprogramming.
This feature becomes critical when your clinic experiences electrical issues. Nobody wants to rebuild patient databases from scratch.
Quality Control During Manufacturing
Request information about in-production quality control. What testing occurs at each manufacturing stage? Quality manufacturers test components before assembly, test subassemblies during production, and test complete units before packaging.
Ask for quality control documentation. Reliable suppliers provide inspection reports willingly. Hesitation suggests weak quality systems.
Regulatory Certification Verification
Different markets require different certifications. For US distribution, FDA registration 8 matters. For European markets, CE marking is essential. For your specific target market, verify which certifications apply.
Do not accept verbal assurances. Request certification documents. Verify registration numbers independently through regulatory databases. Fraudulent documentation exists in this industry.
Service and Support Infrastructure
After-sales support determines long-term satisfaction. Ask about:
- Warranty terms and coverage
- Response time for technical issues
- Parts availability and shipping times
- Training materials provided
- Remote diagnostic capabilities
A manufacturer who disappears after payment creates ongoing problems. Evaluate communication responsiveness during the inquiry phase. Slow responses before purchase predict poor support afterward.
Customization and OEM Capabilities
If you plan to brand devices under your own label, assess OEM capabilities thoroughly. Can the manufacturer add your logo and branding? Can they modify interface language for your market? Will they provide branded user manuals and marketing materials?
Customization extends beyond cosmetics. Software modifications, treatment protocol presets, and accessory configurations may differentiate your offering. Discuss these requirements early in supplier evaluation.
Conclusion
Shockwave therapy offers measurable benefits for postoperative recovery when applied correctly with quality equipment. The evidence supports its use as an adjunctive treatment alongside standard rehabilitation protocols. Your success depends on choosing reliable equipment, understanding proper protocols, and setting realistic patient expectations for treatment timelines.
Footnotes
1. Explains the Lysholm Knee Score, its components, and interpretation for knee function. ↩︎
2. Offers guidance on surgical scar formation, healing timeline, and management. ↩︎
3. Provides a definition and overview of angiogenesis, the formation of new blood vessels. ↩︎
4. Authoritative government source (ClinicalTrials.gov) detailing a clinical study on ACL reconstruction. ↩︎
5. Describes the stages and factors influencing bone fracture healing. ↩︎
6. Authoritative academic source (PubMed) providing a concept analysis and definition of postoperative recovery. ↩︎
7. Defines medical contraindications, distinguishing between absolute and relative types. ↩︎
8. Explains the FDA’s requirements for medical device establishment registration and listing. ↩︎


