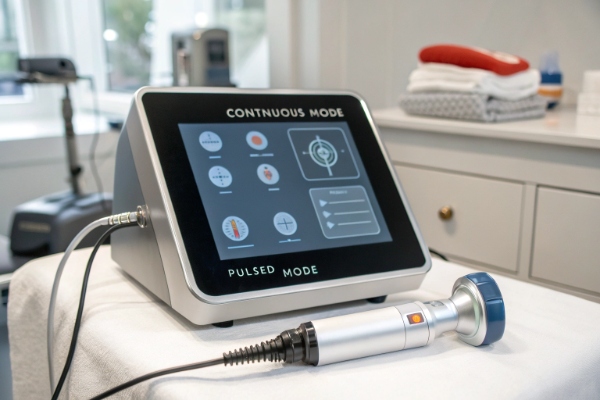
As the manufacturer, I design shockwave systems that combine multiple operating modes to give clinicians the ability to tailor therapy intensity, comfort, and coverage to different patient needs—an approach consistent with how modern extracorporeal shockwave therapy 1 devices evolve for clinical versatility.
Yes. Most professional shockwave therapy machines support both continuous and pulsed (burst or single) modes. Continuous mode delivers uninterrupted shock sequences for fast area coverage, while pulsed mode allows precise, intermittent energy bursts for targeted, patient-friendly treatment.
This dual-mode structure reflects how different tissues respond to varied mechanical energy dosing principles 2, making the device suitable for musculoskeletal, rehabilitation, and aesthetic applications.
Understanding how these modes differ and when to use each helps clinics maximize therapeutic outcomes and equipment lifespan.
How do continuous and pulsed modes differ in therapeutic applications?
Continuous and pulsed operation modes differ in how energy is delivered to the tissue. Each has unique advantages depending on treatment goals and patient tolerance, aligning with documented variations in tissue mechanotransduction response 3.
Continuous mode provides steady, uninterrupted acoustic pulses for uniform coverage, whereas pulsed mode separates energy bursts by intervals, allowing precise targeting and better comfort control for sensitive areas.

Functional distinction
Continuous mode maintains constant frequency, useful for warming tissue or improving local circulation—similar to principles in percussion-based soft-tissue therapy 4. Pulsed mode spaces shocks to give recovery time, reducing perceived intensity and mechanical load.
Table 1 — Functional comparison between modes
| Parameter | Continuous mode | Pulsed mode |
|---|---|---|
| Wave pattern | Unbroken pulse train | Bursts or single shots |
| Thermal load | Higher | Lower |
| Comfort level | Moderate | Higher |
| Target precision | Lower | Higher |
| Typical use | Large-area massage or aesthetic smoothing | Trigger point, tendon, focal lesion |
Continuous operation emphasizes efficiency, while pulsed treatment emphasizes control and comfort.
What treatment indications benefit from each mode type?
Different conditions respond better to specific energy delivery patterns. Selecting the correct mode improves both safety and therapeutic effect and aligns with how clinicians select protocols for tendinopathy management 5 or other MSK conditions.
Continuous mode is ideal for large muscles, fascia, and broad areas requiring circulation improvement. Pulsed mode works best for focal pain sites, chronic tendinopathies, and small treatment zones where comfort and accuracy matter most.

Indication overview
- Continuous: Large muscle groups, general stiffness, cellulite smoothing, chronic low-back tension.
- Pulsed: Plantar fasciitis, tennis elbow, rotator cuff injury, myofascial trigger points, scar remodeling—conditions commonly addressed with noninvasive MSK therapy 6.
Table 2 — Recommended mode selection
| Application | Recommended mode | Frequency | Energy range | Session duration |
|---|---|---|---|---|
| Cellulite therapy | Continuous | 10–20 Hz | Low–Medium | 8–12 min |
| Plantar fasciitis | Pulsed | 6–8 Hz | Medium–High | 5–8 min |
| Muscle relaxation | Continuous | 15–20 Hz | Low | 5–10 min |
| Tendonitis | Pulsed | 6–10 Hz | Medium | 5–8 min |
| Shoulder pain | Pulsed | 6–8 Hz | Medium | 6–10 min |
What should buyers check regarding mode switching and user interface?
Before purchasing, buyers should verify whether the device allows easy and safe switching between emission modes during operation—something emphasized in many clinical device usability and safety frameworks 7.
Buyers should ensure that the interface supports single-touch switching, per-mode presets, and energy ramping to prevent sudden output jumps. The system should also clearly display active mode status to minimize operator error.

What to verify
- Ease of access: Switching modes should not interrupt treatment.
- Preset options: Each mode should have adjustable energy and frequency presets.
- Safety interlock: Automatic soft-start prevents intensity spikes.
- Display clarity: Icons and color codes differentiate modes clearly.
- Session tracking: Systems with pulse counters and logs simplify clinical documentation.
Are there safety implications when changing between continuous vs pulsed modes?
Switching modes changes both mechanical stress and patient perception. Safety depends on the device’s internal control algorithms and the operator’s technique, consistent with general non-thermal ultrasound and mechanostimulation safety principles 8.
Mode changes can affect average power output and thermal load. Certified devices implement ramp-up sequences, thermal monitoring, and auto-adjusted limits to ensure the transition does not cause discomfort or tissue stress.
Typical built-in safety systems
- Soft-start control: Prevents sudden shock intensity increase.
- Thermal sensor feedback: Pauses operation if handpiece exceeds safe limits.
- Firmware safety lock: Reverts to safe energy if parameters mismatch.
- Cooling intermission: Optional delay timer after extended continuous use, similar to common heat-management practices in electro-mechanical devices 9.
Table 4 — Safety comparison between operation modes
| Risk factor | Continuous mode | Pulsed mode | Mitigation |
|---|---|---|---|
| Heat buildup | Higher | Lower | Auto cooling, temperature sensors |
| Mechanical stress | Moderate | Low | Regular maintenance |
| Operator error | Moderate | Low | Clear display indicators |
| Energy drift | Possible | Controlled | Calibration checks |
| Patient comfort | Variable | Stable | Gradual ramping |
When used properly, both modes are safe and effective. Issues arise only when devices lack proper monitoring or operators ignore required cooldown intervals—conditions described in clinical ESWT best-practice guidelines 10.
Conclusion
Continuous and pulsed shockwave modes each have their advantages. Continuous operation treats broad tissue zones quickly, while pulsed delivery offers precision and comfort for sensitive regions.
Machines supporting both allow clinics to tailor each session for the best therapeutic effect and patient satisfaction.
Footnotes
1. Overview of ESWT technology and clinical use. ↩︎
2. Study explaining energy-dose mechanisms in acoustic therapies. ↩︎
3. Research article on cellular response to mechanical stimulation. ↩︎
4. Background on percussion-style soft-tissue therapy principles. ↩︎
5. Review of shockwave therapy in tendinopathy and MSK care. ↩︎
6. Clinical explanation of ESWT for common pain conditions. ↩︎
7. ISO usability and safety framework relevant to clinical devices. ↩︎
8. Research on mechanostimulation safety thresholds. ↩︎
9. Overview of thermal behavior in electro-mechanical medical systems. ↩︎
10. Clinical guideline summarizing safe ESWT operation protocols. ↩︎


